- Home
- Foot & Ankle Conditions
- Sports Injuries
- Posterior Tibial Dysfunction
Posterior Tibial Dysfunction
- Published 11/1/2023
- Last Reviewed 11/29/2023
In this video, we talk about the posterior tibial tendon, its function, injuries, and treatment options.
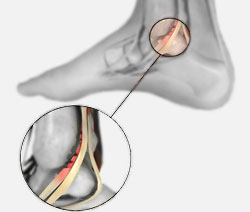
The tibialis posterior tendon attaches the calf muscle to the bones inside of the foot. It passes through the inside of the ankle before continuing up the lower leg. It supports the foot and arch while walking.
Flat feet or constant stress in the midfoot can cause the tendon to fray and tear, resulting in posterior tibial tendon dysfunction (PTTD). The condition is also the most common cause of adult-acquired flatfoot deformity, as the weakening of the tendon causes the arches to fall. About 80% of adult-acquire flatfoot cases are thought to be caused by PTTD.
-
Foot and Ankle Surgeon at University Foot and Ankle Institute
Dr. Abimbola Johnson completed his undergraduate degree at Loyola University Chicago, where he played Division II rugby and was also involved in social justice clubs aimed at helping younger students prepare for college.
Upon graduation, he entered Scholl College of Podiatric Medicine, where he served as president of the practice management club and volunteered as coordinator at the Free Foot Clinic in Chicago. He served his residency at Regions Hospital/Health Partners in St. Paul.
Dr. Johnson provides comprehensive medical and surgical care for a wide spectrum of foot and ankle conditions, including common and complex disorders and injuries. The doctor is uniquely qualified to detect the early stages of disease that exhibit warning signs in the lower extremities, such as diabetes, arthritis, and cardiovascular disease.
Dr. Johnson can be seen at our Santa Barbara location
 Doctor jafary and all the nurses are doing great job and Doctor jafary he is amazing Doctor and they have good customer service...Ibrahim66132 H.
Doctor jafary and all the nurses are doing great job and Doctor jafary he is amazing Doctor and they have good customer service...Ibrahim66132 H. Please provide handicap parkingBarry S.
Please provide handicap parkingBarry S. Dr. Ambibola Johnson is awesome!Laurie S.
Dr. Ambibola Johnson is awesome!Laurie S. The staff was amazing from the start of my visit.Cairo R.
The staff was amazing from the start of my visit.Cairo R. I appreciate the care and timeliness of all my appointments I’ve had at UFAI. Gray, Lydia and the staff all are wonderful. Lydi...Edelmira G.
I appreciate the care and timeliness of all my appointments I’ve had at UFAI. Gray, Lydia and the staff all are wonderful. Lydi...Edelmira G. I had been to another podiatrist for plantar fasciitis and it went of for a year with no relief and painful continuous injectio...Gabe T.
I had been to another podiatrist for plantar fasciitis and it went of for a year with no relief and painful continuous injectio...Gabe T. Very greatfull for the doctor and stuffJesus M.
Very greatfull for the doctor and stuffJesus M. Doctor was very caringBrigitte S.
Doctor was very caringBrigitte S. Everyone is very nice and efficient-
Everyone is very nice and efficient-
Especially Dr Kelman. He takes very good care of me!!Claudia K. Great costumer service.
Great costumer service.
Prompt and efficientDean W. No . I’m pleased with the care .Michael P.
No . I’m pleased with the care .Michael P. Appreciate the professionalism and expertise, as well as the caring.Stella G.
Appreciate the professionalism and expertise, as well as the caring.Stella G.
-
 Listen Now
Bunion Surgery for Seniors: What You Need to Know
Read More
Listen Now
Bunion Surgery for Seniors: What You Need to Know
Read More
-
 Listen Now
Do Blood Pressure Medicines Cause Foot Pain?
Read More
Listen Now
Do Blood Pressure Medicines Cause Foot Pain?
Read More
-
 Listen Now
15 Summer Foot Care Tips to Put Your Best Feet Forward
Read More
Listen Now
15 Summer Foot Care Tips to Put Your Best Feet Forward
Read More
-
 Listen Now
Pediatric Bunion Surgery
Read More
Listen Now
Pediatric Bunion Surgery
Read More
-
 Listen Now
Is Bunion Surgery Covered By Insurance?
Read More
Listen Now
Is Bunion Surgery Covered By Insurance?
Read More
-
 Listen Now
How To Tell If You Have Wide Feet
Read More
Listen Now
How To Tell If You Have Wide Feet
Read More
-
 Listen Now
Bunion Surgery for Athletes: Can We Make It Less Disruptive?
Read More
Listen Now
Bunion Surgery for Athletes: Can We Make It Less Disruptive?
Read More
-
 Listen Now
What To Do When Your Toenail Is Falling Off
Read More
Listen Now
What To Do When Your Toenail Is Falling Off
Read More
-
 Listen Now
Non-Surgical Treatment for Plantar Fasciitis – What Are Your Options?
Read More
Listen Now
Non-Surgical Treatment for Plantar Fasciitis – What Are Your Options?
Read More
-
 Listen Now
Should I See a Podiatrist or Orthopedist for Foot Pain and Ankle Problems?
Read More
Listen Now
Should I See a Podiatrist or Orthopedist for Foot Pain and Ankle Problems?
Read More
-
 Listen Now
Swollen Feet During Pregnancy
Read More
Listen Now
Swollen Feet During Pregnancy
Read More
-
 Listen Now
What Are Shin Splints?
Read More
Listen Now
What Are Shin Splints?
Read More
-
 Listen Now
Top 10 Non-Surgical Treatments for Morton's Neuroma
Read More
Listen Now
Top 10 Non-Surgical Treatments for Morton's Neuroma
Read More
-
 Listen Now
How Many Steps Do I Need A Day?
Read More
Listen Now
How Many Steps Do I Need A Day?
Read More
-
 Listen Now
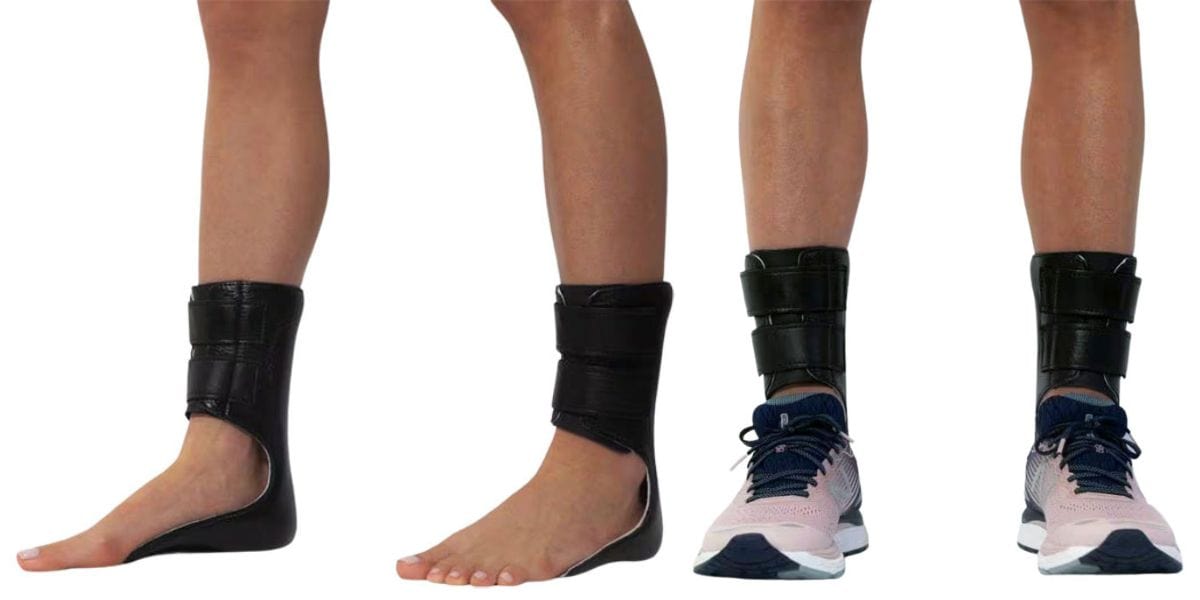
Moore Balance Brace: Enhance Stability and Prevent Falls for Better Mobility
Read More
Listen Now
Moore Balance Brace: Enhance Stability and Prevent Falls for Better Mobility
Read More